Navigating Eosinophilic Esophagitis (EoE): Our Family’s Comprehensive Five-Year Journey and Insights
It will officially be five years next month since my son received his diagnosis of Eosinophilic Esophagitis (EoE), a chronic and often challenging allergic inflammatory disease. Over this significant period, our family has navigated countless appointments, dietary adjustments, and emotional hurdles, ultimately settling into what we now consider our ‘rare disease life.’ Due to the public nature of this blog, I frequently receive heartfelt questions about how we’ve managed this condition. In response, I felt it would be immensely helpful to consolidate our experiences, lessons learned, and practical strategies into one easily accessible resource. This article aims to provide a transparent look into our journey, offering insights that might resonate with other families grappling with EoE or those seeking to understand it better.

*Please be advised that the information shared here is purely based on our family’s personal experience with Eosinophilic Esophagitis. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. I do not assert that our approach is the sole or definitive method for managing this complex disease. My intention is simply to offer a real-world perspective on how one family has navigated EoE, providing potential talking points for you to discuss with your own qualified medical professionals as you determine the best course of care. This post may also contain affiliate links, which help support our mission to share helpful resources.*
What Exactly Is Eosinophilic Esophagitis (EoE)?
Eosinophilic Esophagitis, often abbreviated as EoE, is defined by the American Partnership for Eosinophilic Disorders (APFED), an incredibly valuable organization, as “a chronic, allergic inflammatory disease of the esophagus (the tube connecting the mouth to the stomach). It occurs when a type of white blood cell, the eosinophil, accumulates in the esophagus and persists despite acid-blocking medicine. The elevated number of eosinophils cause injury and inflammation to the esophagus. This damage may make eating difficult or uncomfortable, potentially resulting in poor growth, chronic pain, and/or difficulty swallowing.”
In simpler terms, as I often explain it to others, imagine typical food allergies, but instead of manifesting as skin rashes or breathing difficulties, these allergic reactions primarily affect the esophagus. My son has general food allergies, but due to EoE, his esophagus also reacts allergically to certain foods. When he ingests these trigger foods, it leads to inflammation and damage within his esophageal lining. This internal irritation can cause significant pain, swelling, and in severe cases, even lead to food becoming physically stuck in his esophagus, a frightening event known as an impaction. It’s a persistent battle against internal allergic responses that directly impact one of the most fundamental daily activities: eating.
Identifying the Early Signs: My Son’s EoE Symptoms
One of the most frequent questions I receive revolves around my son’s initial symptoms. Early detection of EoE, especially in infants and toddlers, can be incredibly challenging as symptoms are often non-specific and can mimic other common childhood ailments. Around two months of age, we started noticing significant, bright red rashes on my son’s cheeks shortly after breastfeeding sessions. Concurrently, his bowel movements became highly problematic: they were consistently runny, contained mucous, and often resulted in “blowouts” after almost every diaper change. He also experienced what I can only describe as “machine-gun-like” gas. While these individual issues, like diaper problems, don’t always signal a serious underlying condition, their persistent combination raised concerns for us.
Initially, his pediatrician suggested an immature immune system was likely the culprit, recommending I undertake an elimination diet since he was exclusively breastfed. What surprised me was the specific assortment of foods she advised me to remove: dairy, nuts, eggs, whole grains, citrus, corn, strawberries, tomato, and chocolate. These weren’t the standard top-8 allergens, making the diet quite restrictive. I eliminated all these items for two weeks to clear my system, then reintroduced them one by one, starting with chocolate and working backward. Each food was eaten for three days, and if my son showed no adverse reactions, it was deemed safe to remain in my diet. Through this meticulous process, we identified eggs, soy, and wheat as triggers, which I diligently avoided throughout the year I breastfed him.
As we transitioned him to solid foods, new and concerning patterns emerged. He displayed a distinct disinterest in eating, frequently vomited, and the troublesome cheek rashes often reappeared. Most alarmingly, his weight percentiles began to plummet, placing him almost entirely off the growth curve by the time we finally secured an appointment with an allergist. These escalating symptoms painted a clear picture that something more significant than typical infant issues was at play, driving us to seek specialized medical attention.

The Diagnostic Journey: How and When My Son Was Diagnosed with EoE
The definitive and only official method for diagnosing Eosinophilic Esophagitis involves an Esophagogastroduodenoscopy (EGD), commonly referred to as an endoscopy or “scope,” accompanied by biopsies. During this procedure, tissue samples are taken from the esophagus, stomach, and duodenum. These biopsies are then meticulously examined by a pathologist under a microscope to confirm the presence and elevated number of eosinophils within the esophageal tissue, which is the hallmark of EoE.
By eleven months of age, my son had experienced an anaphylactic reaction to his first exposure to dairy. Coupled with his history of reacting to eggs, soy, and wheat through my breast milk, his allergist decided to conduct blood work. The results were startling: his blood eosinophil count was exceptionally high. The allergist candidly stated that this could indicate either EoE or even leukemia, emphasizing the urgent need for an EGD. It’s crucial to understand that while elevated blood eosinophils can be a strong predictor, blood tests alone are not diagnostic for EoE. The only way to truly understand what’s happening at the tissue level in the esophagus and obtain a definitive diagnosis is through direct tissue samples obtained via biopsy during an EGD.
Since allergists do not perform EGDs, we were referred to a pediatric gastroenterologist. Following the procedure, the pathologist’s confirmation of eosinophil presence in his esophageal tissue led to his official diagnosis of EoE at 14 months old. This journey highlights the multi-specialty approach often required for managing complex conditions like EoE, underscoring the importance of close collaboration between allergists and gastroenterologists.
Life After an EGD (Scope): Our Child’s Experience
A common concern for parents of children with EoE is how their child copes with repeated EGD procedures. In our experience, my son has generally done remarkably well after his scopes. I believe he possesses a naturally high pain tolerance, and the procedures themselves, while invasive, are not inherently the “worst” experiences. They are relatively quick, typically lasting only about 15 minutes while the child is under anesthesia. I’ve been told by medical staff that the instrument used to take the tiny tissue samples is about the size of the tip of a pen, which helps put the invasiveness into perspective.
Of course, the level of discomfort can vary depending on the extent of esophageal damage, the number of biopsies taken, and the time elapsed since the last procedure. There was one instance where the doctor mentioned his esophagus was quite fragile, resulting in some bleeding after a sample was taken. This led to my son vomiting blood on an empty stomach when he awoke from anesthesia, which was certainly distressing for us to witness. However, such incidents have been rare. To aid recovery, he is always given fluids before leaving the hospital, and we typically offer soft foods for about a day afterward. Beyond a dose of Tylenol, which he sometimes doesn’t even request, he recovers quickly and is usually back to his usual self.
The Challenge of Uncovering EoE Triggers: Our Approach
Identifying EoE triggers can feel like searching for a needle in a haystack—it’s incredibly complex and demands immense patience. The recommended methodologies have also evolved since we first embarked on this journey. Nevertheless, here’s an in-depth look at how we approached trigger identification for our son.
Our allergist at Primary Children’s Hospital in Salt Lake City initially followed the Cincinnati Children’s Hospital’s recommendations (Cincinnati being one of the leading EoE clinics alongside Denver) for patch testing. This meant that at least twice a week, and sometimes more frequently, we would drive 45 minutes each way for appointments. The process began with prick testing to rule out any immediate, anaphylactic reactions to a food. If he passed the prick test, we would then proceed with patch testing. My son has undergone testing for well over 100 foods (I lost count after 100), as we were advised that virtually every single food he might ever consume needed to be tested. It was an incredibly long and arduous period, with my poor son spending the majority of his second year of life in a doctor’s office. He became so accustomed to the prick tests that they no longer bothered him; he wouldn’t even flinch—a true testament to his trooper spirit.
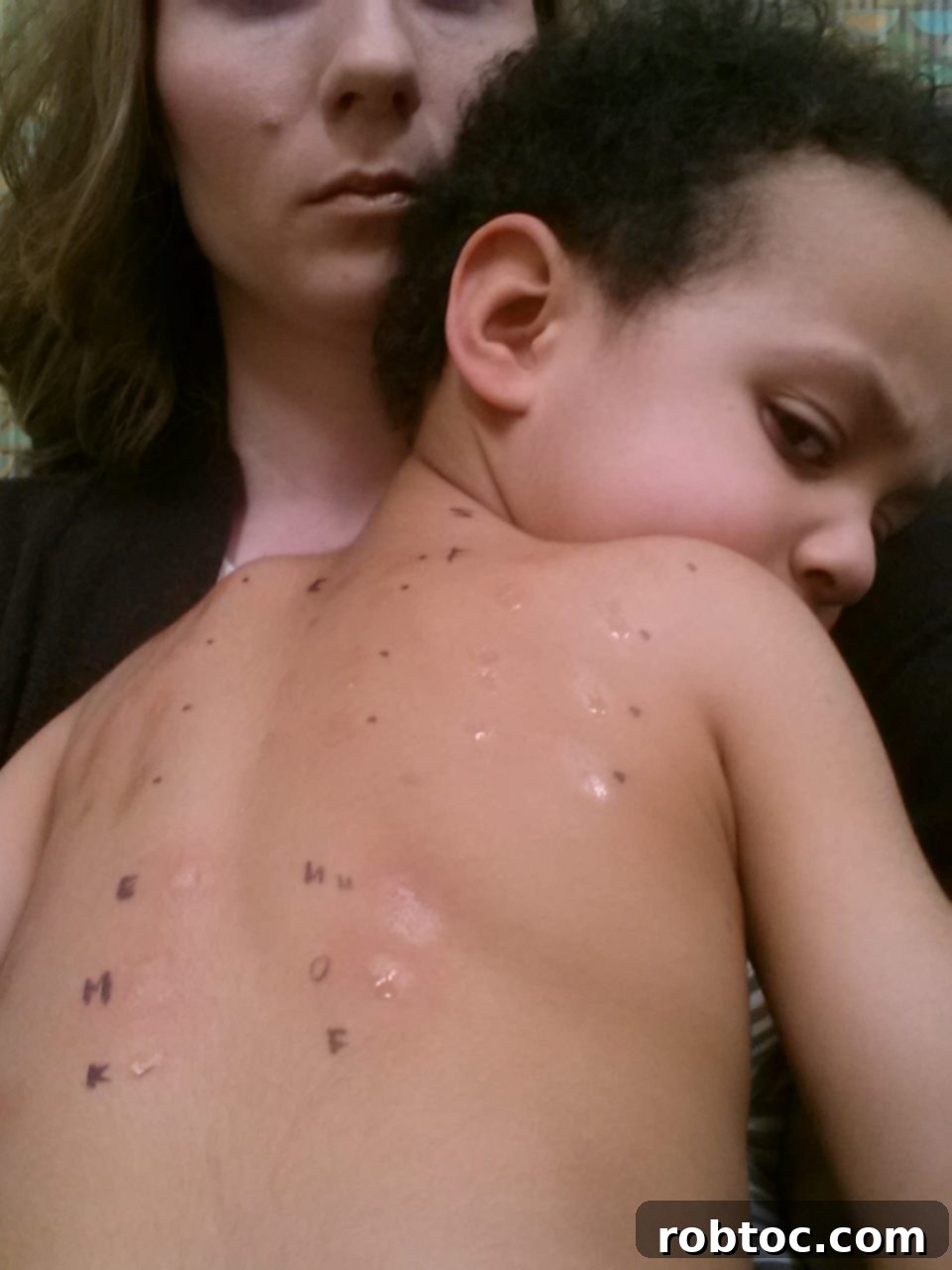
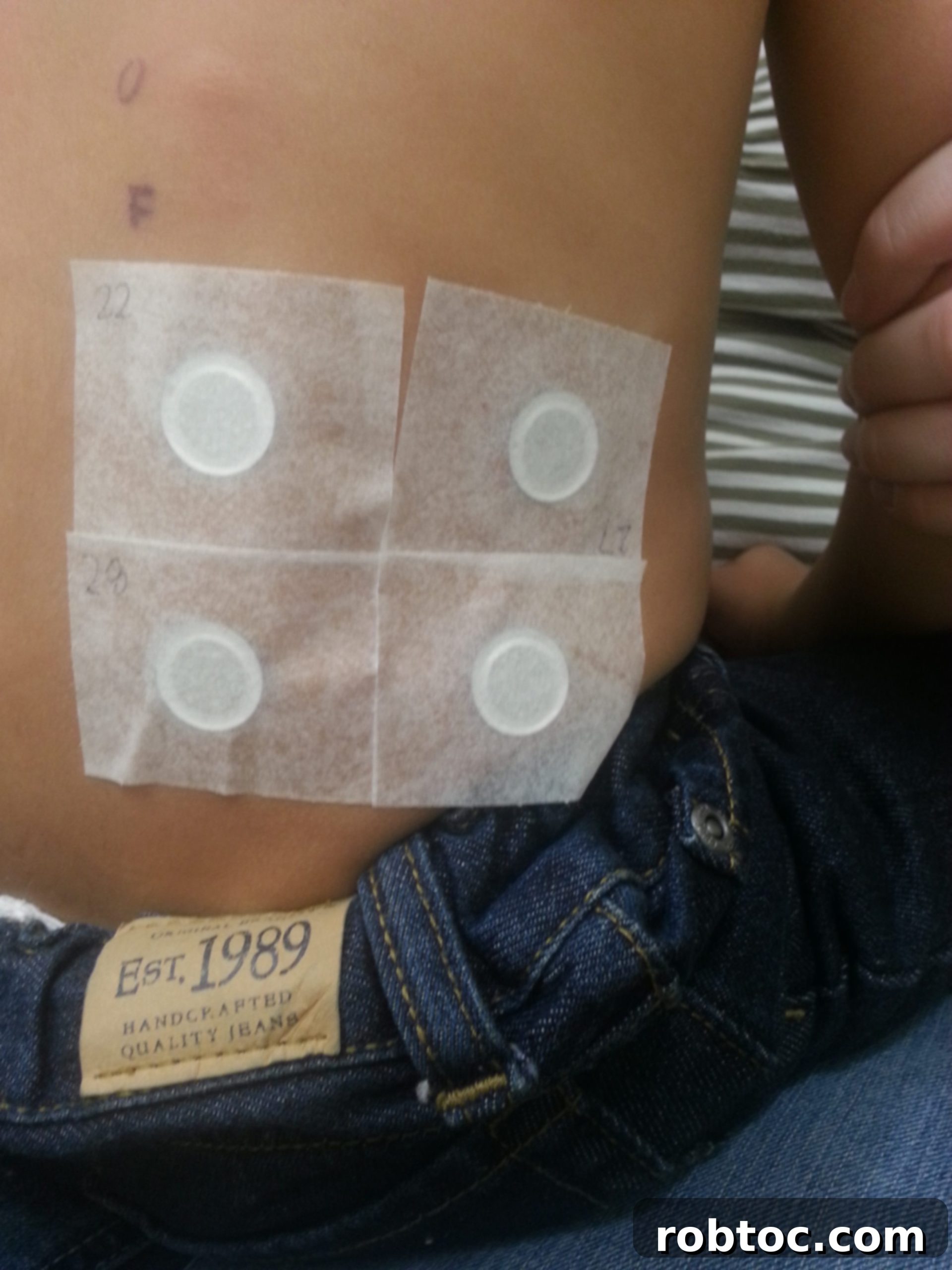
For those unfamiliar with patch testing (also known as atopy patch testing), it involves creating a paste from the actual food (the exact food-to-saline proportions were never disclosed to me), placing a small amount on a disc, and then taping that disc to the child’s back. A control disc with just saline was always included, alongside discs with various food proteins. I would often bring grocery bags full of foods that weren’t readily available in the clinic, and our allergist allowed me to prioritize which foods and in what order we tested them, based on what I cooked with most frequently.
The underlying premise of patch testing was to observe how the skin tissue would react to prolonged exposure to food proteins, attempting to mimic the slower, delayed reactions often seen in the esophagus. These patches, held firmly in place by a considerable amount of tape, had to remain on his back for two full days. We even continued this rigorous process throughout the summer months. My son, incredibly resilient, could not swim or bathe during these periods and showed remarkable restraint in not scratching the patches. Ironically, his biggest cries often came when I had to remove the patches, as the tape would pull on his fine back hairs. It was a moment I dreaded, often bringing tears to both our eyes—those truly were challenging months.
After two days, I would carefully remove the patches at home, meticulously taking photographs of any skin reactions (some doctors require patients to return to the clinic for removal, but our doctor trusted my handling). The skin was then allowed to air out for another day, again without bathing. Finally, on the third day, we would return to the clinic for the “reading” of the results. Any raised skin, redness, or irritation at the patch sites was considered a “fail,” indicating a potential trigger.
If my son successfully passed both the prick and patch tests for a food, he was then permitted to try it orally. While he had consumed many fruits and vegetables in pureed form as an infant, this re-testing process gave us greater confidence that these foods were “safer” and less likely to trigger his EoE and cause esophageal damage. Despite his previous exposure to a decent number of foods, we re-tested EVERYTHING to avoid assumptions, given that whatever he had been eating previously was causing internal damage.
To maximize each appointment, we would fill his back with as many patches as possible. When he passed any foods (there were disappointing failures every time, making those 45-minute drives home particularly hard, often leading me to call my mom or best friends for a cry), we would then allow him to eat that single, newly cleared food once a day for several weeks. During this oral trial phase, we carefully monitored for any reactions on his skin, in his bowel movements, changes in eating habits, or instances of vomiting. This meticulous tracking was done for each food he passed.
Thankfully, we only encountered one instance during the oral trial stage where a food seemed to affect him negatively: green beans, of all things. They caused him severe constipation, so we deemed it a fail and did not pursue further testing or scoping for that particular food.
It’s important to note that most current medical literature and guidelines generally do not recommend prick or patch testing for EoE, as many studies indicate a poor correlation with esophageal inflammation. However, for our family, I genuinely felt it was helpful, particularly because patch testing is reported to have a higher success rate in children than adults. For example, he had a horrific reaction to mustard, a food we never would have suspected. After several years of strict avoidance, we cautiously reintroduced it, and he spent days clearing his throat and coughing persistently. That said, I believe we were among the lucky few for whom it yielded useful information, as most families I’ve spoken with did not find it beneficial. In hindsight, not doing it would have saved us considerable time and hassle, but at the time, we were following what was considered cutting-edge advice (though I often wondered, who first thought of taping food to someone’s back?).
Strategies for Scoping: Testing Multiple Foods Simultaneously
A frequently asked question concerns our approach to scoping multiple foods at once. Yes, we did scope to more than one food simultaneously, a decision we understood carried inherent risks. The primary gamble was that if the scope revealed inflammation, we wouldn’t know which specific food among the tested group was the culprit. However, after much prayer, relying on a mother’s intuition, and meticulously calculating our approach, by the time we reached the stage of scoping foods my son was regularly eating and seemed to tolerate well, we felt confident in his progress. We sought the scopes primarily for confirmation, believing we had already successfully identified and eliminated the problematic foods. This strategy made sense for us because his list of safe foods was still quite limited. While there’s absolutely nothing wrong with a slower, one-food-at-a-time scoping approach, we made a personal decision to take this calculated risk given our specific circumstances.
Another critical consideration we factored into our scoping schedule was the time of year. We always made an effort to avoid scheduling scopes during high pollen seasons. There’s a prevailing idea within the EoE community that swallowing environmental allergens like pollen can also trigger an esophageal reaction and inflammation. Therefore, we preferred to wait until winter months when pollen levels are significantly lower, allowing us to rule out that potential confounding factor and get a clearer picture of food-induced inflammation.
The Pillars of Support: What Helped Us Most in Our EoE Journey
Without a doubt, the most crucial elements that supported us through our EoE journey were unwavering support and readily available knowledge. We were incredibly fortunate to assemble an excellent medical team. Our allergist specialized specifically in EoE, and our GI doctor was part of the same Primary Children’s Hospital system, facilitating seamless communication and collaboration between them. This integrated care was invaluable. We also had the guidance of a fantastic dietitian (more on her later!) who became an indispensable resource.
Beyond the medical professionals, our network of friends and family provided immense emotional support. They were willing to sympathize, listen to my cries during those long, stressful drives home, and even alter their meal plans during get-togethers to accommodate my son’s dietary restrictions, which meant the world to us. I actively sought out and joined two local support groups: one specifically for EoE and a general food allergy group (Utah Food Allergy Network) that hosted yearly conferences. These groups allowed me to connect with other mothers who had been managing EoE for longer, providing a safe space to bounce ideas, share frustrations, and gain practical advice. I also expanded my network by joining several online support groups on Facebook, enabling me to ask questions to a broader audience and benefit from diverse experiences.
Crucially, my faith in God and His purpose and plan for my family provided an enduring source of strength. Without this spiritual foundation, I honestly believe I wouldn’t have made it through so many disheartening and overwhelming times. It offered perspective and hope when things felt most challenging.
The Indispensable Role of a Specialized Dietitian for EoE
I cannot stress enough the recommendation for involving a dietitian in the management of EoE, especially for pediatric patients. However, it’s vital to understand that not all dietitians possess the specialized knowledge required for such a complex condition. We proactively sought out a dietitian who was highly experienced with pediatric patients facing severely limited diets. This distinction was critical; she never questioned “why” my son was down to only ten foods but instead was wholly focused on “how” he could meet his daily nutritional requirements despite these restrictions.
Her approach was incredibly thorough and reassuring. She had me maintain a detailed food diary for three days, meticulously recording every ingredient and its quantity that my son consumed. From this data, she would calculate his intake of essential nutrients such as iron, protein, and various vitamins. She then identified any deficiencies and collaboratively devised strategies to address them, whether through multi-vitamins, iron supplements, fortified rice milk, or simply increasing the quantity of safe foods. This rigorous monitoring provided immense comfort, knowing that even with his severely restricted diet, my son was still growing (she would weigh and measure him in just his underwear at every visit) and receiving adequate nutrition. This peace of mind was invaluable during an otherwise stressful period.
Considering a Feeding Tube: Our Son’s Close Call with EoE
While my son never ultimately required a feeding tube due to EoE, we came very close, and it’s a common consideration for many patients, particularly those on elemental formula. When his safe food list dwindled to a minimal number, the use of elemental formula—a specialized, hypoallergenic liquid diet common among EoE patients—was suggested. At that time, I was fiercely determined, perhaps for some misguided reasons (as I now recognize the immense help these can provide), to spend my time in the kitchen creating safe meals rather than resorting to a feeding tube.
Thanks to our dedicated dietitian, we realized that despite the limitations, he was maintaining his health. Our continuous efforts in testing and gradually adding foods to his diet—from ten, then twenty, and eventually fifty safe foods!—gave us confidence he would be okay. Furthermore, given his age and the fact he had been breastfed for so long, we knew he would likely refuse the elemental formula orally due to its notoriously unpleasant taste, making a feeding tube a probable necessity if we went that route. I’m grateful we didn’t have to put him through that particular challenge. However, my perspective on feeding tubes underwent a significant shift after a conversation with an older friend who had long suffered from severe eating problems. She wisely observed that if eating itself becomes a tortuous process filled with pain and hassle, a feeding tube can truly be a Godsend. I understand there’s often a stigma associated with them, and I once shared that sentiment myself, but I now firmly believe there is a legitimate time and place for their use as a vital medical intervention.
Ensuring Adequate Calorie Intake on a Restricted EoE Diet
The simple answer to ensuring my son received enough calories on his restricted diet involves three key strategies: consistent consultation with our dietitian, blending his food, and liberal addition of healthy oils. Our primary focus was to incorporate anything extra fatty into his diet. This meant opting for full-fat coconut milk, and choosing fattier cuts of meat like chicken thighs and dark meat over leaner chicken breasts – essentially the opposite of a typical weight-loss diet! As I’ve mentioned elsewhere, blending his food was a game-changer. It allowed us to combine nutrient-dense items like black beans, chicken, asparagus, and brown rice into a single sitting. As a toddler, he definitely wouldn’t have eaten these items individually due to texture or preference. Crucially, we would always add at least a tablespoon of olive oil to these purees to significantly boost the caloric content, ensuring he met his daily energy needs for growth and development.

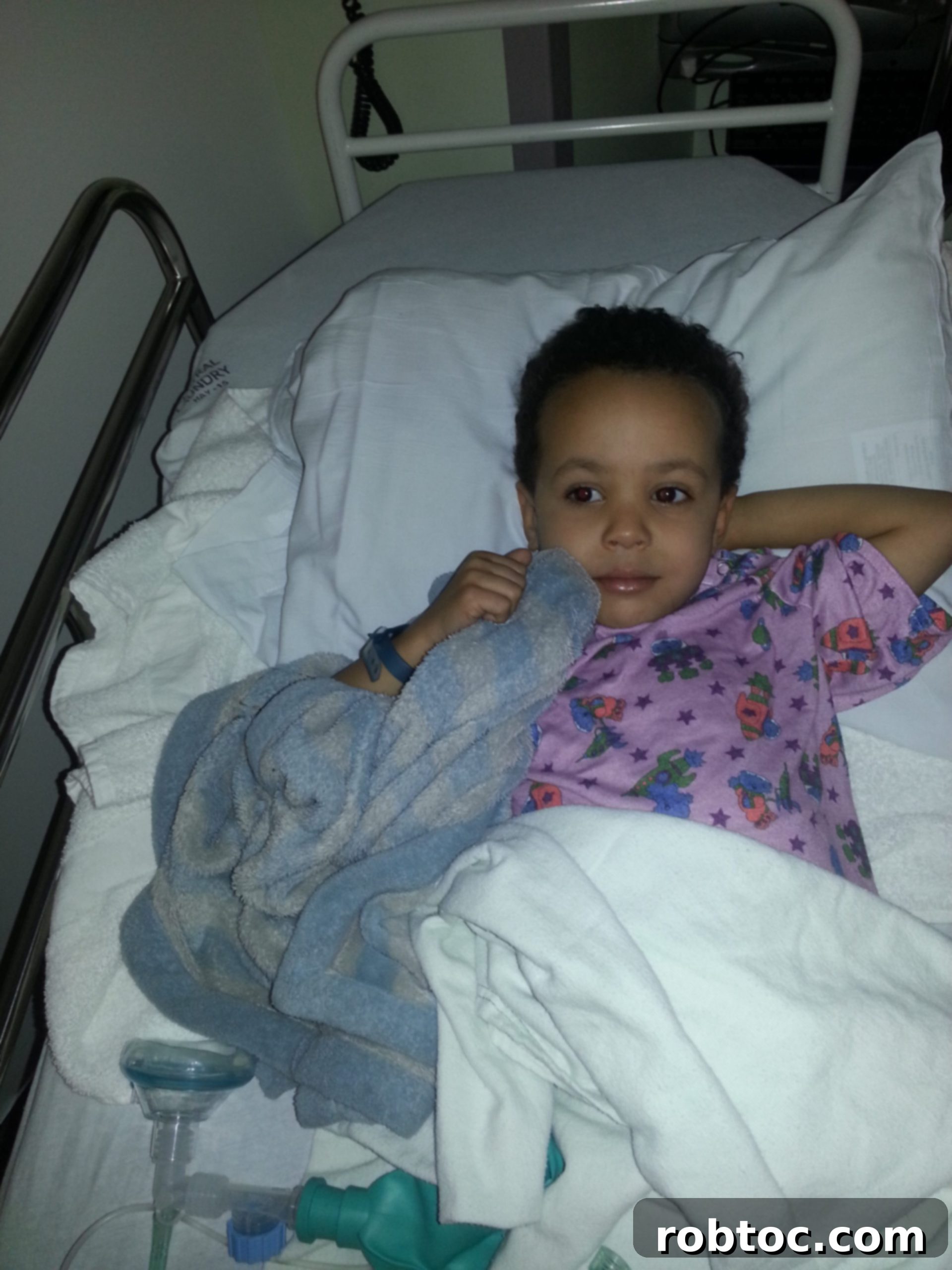
Waiting to be taken back to surgery for his next scope.
The Advantages of Early EoE Diagnosis
Without a doubt, I am absolutely glad we pursued and achieved an EoE diagnosis for my son at such a young age. One of the profound benefits was that he didn’t develop a full awareness of eating “differently.” As a toddler, he hadn’t yet acquired a broad taste for various foods, so he didn’t perceive the loss when certain items were removed from his diet. He simply accepted what was offered. Every year, as he grows older, he becomes more socially aware of what others are eating, which naturally brings its own set of challenges. Receiving the diagnosis early felt like a blessing in disguise because it allowed us to establish his safe diet and management strategies before social pressures and peer comparisons became a significant factor.
Furthermore, as he was our first child, I had the luxury of dedicating ample time and energy to understanding EoE and meticulously figuring out his triggers and dietary needs. This focused effort during his crucial early years laid a solid foundation for his health management before our other children came along, making the overall process more manageable for our growing family.
Determining Scope Frequency: Our Evolving Approach to Monitoring EoE
The recommended frequency for endoscopic monitoring (scopes) in EoE patients varies widely, and I’ve heard every conceivable suggestion. In the initial years, we typically scheduled a scope approximately every six months, or whenever we felt we had a sufficient number of foods ready for oral trial and subsequent assessment. As my son’s diet stabilized and fewer new foods were being introduced, we transitioned to an annual scoping schedule.
However, my son has now undergone six scopes, and as he grows older, he has begun to express a strong desire for a break from these procedures. This has prompted us to consider extending the interval between scopes to two years. Our reasoning behind this is multifaceted: we want to empower him to advocate for his own health, and we feel it would be contradictory to teach him advocacy while simultaneously disregarding his heartfelt requests. Of course, if his health showed any signs of deterioration or increased symptoms, we would immediately schedule a scope. But given his current stable condition, we feel comfortable with this extended interval. It’s important to acknowledge that this is a highly personal decision for each family, and also a financially significant one, as scopes are expensive procedures.
The Invaluable Role of Eosinophilic Esophagitis Support Groups
Joining a support group for Eosinophilic Esophagitis is something I absolutely recommend. These communities can be an invaluable source of information, empathy, and practical advice from others who truly understand the daily challenges of living with EoE. However, it’s equally important to approach these groups with a balanced perspective and use them judiciously. Some members naturally use these platforms to vent frustrations and complain, which can be necessary and cathartic at times. But during an already difficult period, it’s crucial to ensure that you are also actively filling your life with positivity and constructive engagement. Seek out those who offer encouragement, share successes, and provide actionable tips, helping you to maintain a hopeful and proactive mindset while still acknowledging the difficulties. Finding your tribe, whether in person or online, can make a profound difference in your ability to cope and thrive.
Distinguishing Between Anaphylaxis and EoE Food Avoidance
This is a critical distinction that often causes confusion, especially since my son manages both anaphylactic food allergies and EoE food triggers. We approach the avoidance of these two types of allergens with very different levels of caution.
For his anaphylactic foods, such as dairy, avoidance is absolute and non-negotiable. This means strict adherence to no cross-contact whatsoever. For example, you cannot use the same knife, cutting board, or utensil to prepare an unsafe food and then use it for his food, because even trace amounts can provoke a life-threatening reaction that necessitates an EpiPen and immediate emergency medical attention.
In contrast, with EoE triggers, while I remain careful and vigilant, the reaction profile is generally different. If he were to accidentally ingest a trace amount of an EoE trigger on a single occasion, it typically doesn’t cause an immediate or severe symptomatic reaction. Again, this can vary dramatically from patient to patient, and often between adults and children, as symptoms can present differently across age groups. I’ve heard accounts of some individuals experiencing an impaction (where food gets stuck in the esophagus) from a single accidental ingestion, while for others, it takes multiple exposures and a slow build-up of inflammation over time before symptoms become noticeable. Some adults even report “cheating” on their diet occasionally for special events, something we would never risk with anaphylactic allergens.
For instance, my son should ideally avoid pepper due to it being an EoE trigger for him. But if we dine out and I notice a small amount of pepper on his food – which often happens because people season food reflexively – we will typically allow it. Since dining out is a rare occurrence for us, these infrequent, trace exposures have never caused him a discernible problem. The key difference lies in the immediate life-threatening nature of anaphylaxis versus the chronic, inflammatory, and often delayed impact of EoE. This delayed reaction is also a double-edged sword: while it grants some leeway with trace amounts, it also means a food might seem safe for a while before enough inflammation builds up for symptoms to appear, making ongoing vigilance essential to identify new triggers or confirm old ones.
What Foods Can My Son Eat? Unveiling His Specific EoE Triggers
Many readers are curious about the specifics of my son’s diet. To keep this article focused on the journey and management, I maintain a dedicated resource on my website. You can find a comprehensive and regularly updated list of his safe and unsafe foods there. This list is a living document, reflecting our ongoing discoveries and adjustments as we continue to manage his EoE and anaphylactic allergies.
Alleviating EoE Flares: Our Experience with Symptom Management
During our five-year journey, my son has only experienced one significant EoE flare where he felt something was genuinely stuck in his esophagus and was visibly distressed. Occasionally, he might exhibit some throat clearing, but this symptom has never persisted or escalated into a major issue. I’ve heard from other parents that medications such as Ibuprofen, Maalox, Pepcid, or Zantac can help manage stomach pain during flares. Additionally, swallowed Flovent, which my son already has on hand for his asthma, is sometimes used to ease esophageal symptoms by coating the inflamed lining.
However, I must emphasize that managing flares and prescribing medication is definitely a question for your doctor. As a parent, I am not qualified to offer medical advice or treatment recommendations. Always consult with your medical team to determine the appropriate course of action for your child’s specific symptoms and needs during an EoE flare.
Steroid Treatment for EoE: Our Family’s Decision
The use of swallowed steroids is a common management strategy for many individuals with Eosinophilic Esophagitis, particularly adults. My uncle, interestingly not a blood relative but through marriage, is one such person who manages his EoE with swallowed steroids. The principle behind this treatment is that as the steroid medication is swallowed, it coats the esophagus, helping to reduce inflammation and heal the damage caused by food or environmental allergens. Many patients choose this route either as their primary treatment or to avoid drastic dietary changes.
For our son, personally, I felt uneasy about putting him on daily swallowed steroids at such a young age. We had learned about a potential impact on the adrenal system, and given that EoE is a relatively new disease with unknown long-term effects of steroid use in children, I didn’t feel comfortable with this option. Therefore, we made the conscious decision to manage his condition primarily through rigorous dietary control. That said, I readily acknowledge that if diet modification hadn’t yielded positive results, our decision might have been different. EoE is such a complex and highly personalized disease that one cannot fault how other families choose to cope with it.
Following my son’s very first scope, which confirmed his diagnosis and revealed extensive damage (the doctor provided us with pictures each time), we did, however, put him on a two-week course of a swallowed budesonide slurry. This involves mixing liquid budesonide with sugar to make it easier to swallow, though one must then be vigilant about monitoring for candida (yeast infection). This short-term steroid regimen was prescribed to accelerate the healing of his esophagus, as at 14 months old, he was barely on the growth chart and eating very little. Although he was too young to verbalize his discomfort, his persistent refusal to eat was a clear indicator that he wasn’t feeling well. He was, in fact, a remarkably happy baby, so much so that one wouldn’t suspect he had such a debilitating disease. We concluded that he was simply so accustomed to feeling unwell that he didn’t know any different, necessitating our reliance on subtle cues like food refusal to gauge his health.
EoE’s Impact on Development: Our Son’s Growth Journey
For us, yes, having EoE did impact other areas of my son’s early growth and development. He experienced delays in crawling, walking, and speech. Consequently, he underwent various therapies for all these areas, in addition to feeding therapy. Given his young age at the time, it’s difficult to definitively say whether these delays were solely due to EoE, or if he would have been delayed anyway, or if the constant feeling of being unwell significantly hampered his developmental progress. What I can confidently share, however, is that he has completely caught up. He is now thriving in mainstream school with no difficulties, excelling in sports, and performing well academically. This is a message of hope to any parent with a young child who might be experiencing developmental delays related to EoE: with dedication and intervention, catch-up is absolutely possible!
When Your Doctor Doesn’t Take EoE Concerns Seriously: Advocating for Your Child
If you suspect your child might have Eosinophilic Esophagitis but feel your pediatrician is not fully acknowledging your concerns, my primary suggestion is always to start by openly communicating with your pediatrician. However, if your concerns continue to feel invalidated, and you genuinely believe there are significant issues at play, you absolutely have the right—and often the necessity—to seek a specialist directly. This is precisely what we did.
We were met with dismissive comments like, “Well, some kids are just small,” or “He sleeps fine and is so happy, he’s probably fine,” and similar reassurances. But this is precisely what a mother’s intuition is for. I am profoundly glad I pressed the issue and fiercely advocated for my son, even though confrontation is something I typically shy away from. One strategy that significantly helped me be taken more seriously was meticulously journaling his symptoms, keeping a detailed food diary (as mentioned earlier), and arriving at appointments with a prepared list of specific questions. When medical professionals observed that I wasn’t merely offering general complaints but was serious, informed, and organized, it helped them realize that there might indeed be more going on than a first-time, worried mom overthinking things. Empower yourself with information and persistence.
Coping with Overwhelm: Managing Diet, Lifestyle, and Emotions with EoE
I won’t deny that I was fortunate to have my first child be the one diagnosed with EoE, as it allowed me to pour an immense amount of time and energy into figuring out his condition. It undeniably consumed me, and I allowed it to bother me deeply for a long time.
One of the most profound pieces of advice I ever received was the importance of grieving the loss of foods. I distinctly remember the moment I learned he couldn’t have spinach anymore. This was during the peak of the spinach craze—spinach smoothies were incredibly popular, and it was touted as a “superfood.” I went home after he failed the patch test for spinach and just bawled. Bawling over spinach! Who would have thought such a thing was possible? But when foods are taken away one by one, each one feels incredibly precious. It’s vital to allow yourself to feel these emotions, to sit with them, and let them pass through you, rather than bottling them up. This is easier said than done, and it’s something I continue to work on.
I believe one of the most effective strategies for managing the emotional toll of EoE is to find your “tribe.” If your immediate friends and family don’t fully grasp the complexities and emotional weight of the condition, seek out those who do. Utilize online communities like Facebook groups, search by hashtags, or inquire at doctors’ offices to connect with people, whether near or far, who can validate your experiences and offer genuine understanding. I found an invaluable in-person support group in Salt Lake City, and attending APFED conferences, both virtually and in person, has also been incredibly beneficial. Above all, do NOT neglect self-care. You must take care of yourself to effectively care for others. And one profound lesson I wish I had learned much earlier is the power of surrender. I only truly grasped its significance recently and highly recommend this podcast episode (and many others by the same author) to any stressed-out momma. It helped me shift my perspective and realize I didn’t have to be a victim of my circumstances.
Approaching Dietary Changes: Slow and Steady Wins the Race
When making dietary changes for EoE, a slow and steady approach is absolutely crucial. Our pediatric GI explicitly instructed us not to change anything before the very first scope. Why? Because if we altered his diet beforehand, there would be no way to accurately assess the baseline inflammation and understand what foods might be contributing to the problem. I often hear people suggest making multiple changes at once and think, “Oh, no! How will you ever know what caused an improvement or worsening if you change more than one variable?”
This need for meticulous, controlled changes is arguably one of the most frustrating aspects of EoE management. For instance, if a scope reveals inflammation, and you simultaneously change the child’s diet and introduce PPIs (proton pump inhibitors, which are thought to help with inflammation and address any concurrent acid reflux), how will you discern whether the improvement came from the dietary changes or the medication? It becomes impossible to isolate the true effective intervention.
Even though we sometimes grouped a few well-tolerated foods for a single scope, we always introduced any *new* food one at a time. We meticulously tracked its effects before ever moving on to another. We only scheduled scopes when we were fairly confident he would pass, primarily seeking internal confirmation that what we observed externally (lack of symptoms) matched the internal state of his esophagus, as that’s the only way to be truly sure.
A vivid example of this slow process occurred after our initial efforts to restrict his diet down to about ten “safe” foods. We fully expected an improved scope result, but to our devastation, it was worse! I thought for sure we would have to eliminate virtually all foods. However, by carefully reviewing his food journal, we noticed a pattern: he frequently developed rashes after I gave him spinach smoothies. It then clicked that I had started incorporating spinach into almost all his blended foods (as he was still mostly on purees at that time). This explained why his scope was worse—instead of having an offending food occasionally, he was consuming it EVERY DAY. Once we eliminated spinach and scoped again, his esophagus was clear. This experience underscored just how important detailed food journals are; it’s incredibly difficult to keep track of everything and recall past consumption without them.
Establishing the Initial Baseline Diet: What We Cut Out First
Honestly, the specific details of how we decided on the original foods to cut out are a bit hazy now, as it was largely doctor-driven. I remember our medical team asking me to list what he had been eating frequently up to that point, and we used that as a baseline to identify common allergens. From there, we aimed to establish a diverse, yet limited, foundational diet. This involved selecting items like rice for a whole grain, chicken as a protein source, black beans for another protein, carrots for a vegetable, and apples for a fruit, along with a few other carefully chosen items. Thankfully, he scoped clean to this initial base diet, which became our safe starting point. From there, we embarked on the long process of testing additional healthy foods that we believed would broaden his diet, that he would enjoy, and that would be seasonally available or easy for me to source year-round. I was also sure to test a variety of spices early on, ensuring that if we were limited to eating chicken constantly, we could at least flavor it differently to maintain some culinary interest.
Strategies for Managing a Limited Diet: Making It Work for a Child with EoE
Successfully maintaining a consistent, limited diet for a child with EoE requires specific strategies, and my son’s age was a significant advantage in our case. Since he was just over a year old at diagnosis, he was already accustomed to bland foods and purees. This early exposure meant he didn’t have established preferences for a wide variety of flavors or textures, nor the social awareness to realize his diet was “different.” This is precisely why I devoted so much intensive time and effort early on to meticulously figuring out his dietary needs before he developed a stronger social recognition of food variety.
To make his limited diet palatable and nutritious, we invested in a high-quality Blendtec blender. This proved to be a lifesaver, allowing us to combine all his safe foods into smooth, chunk-free smoothies or purees. It was also instrumental in discreetly incorporating nutrient-rich vegetables like broccoli and asparagus (some of the first green veggies he tolerated) into his diet, ensuring he received adequate nutrition without having to contend with challenging textures or the visual appeal of certain foods. Again, the strategic use of a variety of spices has been an enormous help, enabling us to create different dry rubs or simply sprinkle seasonings to vary the flavor profiles of his limited meals. If you aim for more dietary options, be prepared for a fast-tracked process of food trialing and scoping as frequently as your medical team recommends, always adhering strictly to proper procedures.
Key Components of Our EoE Food Journal
Keeping a detailed food journal was absolutely critical in identifying my son’s EoE triggers and monitoring his progress. I created a simple, homemade journal using Excel, which allowed for easy customization and tracking. For each entry, I would record the date, specific meal times, and a comprehensive list of everything he ate, including every ingredient. I also marked whether he consumed a particular food more than once that day, which helped us gauge his total intake of various items.
Crucially, the journal included dedicated sections to log any observed reactions. I would note whether he experienced any type of skin reaction (like rashes), bowel reaction (such as diarrhea or constipation), or throat reaction (difficulty swallowing, frequent throat clearing). Any instances of vomiting were also meticulously recorded. Finally, an additional box was reserved for any miscellaneous or unusual reactions we noticed. This systematic approach allowed us to identify patterns and correlations between specific foods and his symptoms, providing invaluable data for our medical team and guiding our dietary decisions.
You Can Do This: A Message of Hope and Resilience
To every parent embarking on or navigating this challenging EoE journey: absolutely, you can do this. I promise you, while it will undoubtedly feel incredibly hard at first, you will adjust. Your child can still thrive, grow, and lead a happy life. And I promise that, over time, this overwhelming feeling will subside. Grant yourself and your family grace, and allow for an adequate adjustment period. One phrase I constantly tell myself and my son is, “We can do hard things.”
One of the many profound benefits of having access to a specialized facility like Primary Children’s Hospital is the perspective it offers. Witnessing the vast array of diseases and hardships other children face provides crucial context. When I feel the urge to cry about my son facing his seventh scope, I look around and see children missing limbs, or those unable to walk. This helps to put things in perspective. My son may have to eat differently, but he can run, jump, speak, and do so much. We genuinely lead a very happy life, and you can too. Hang in there! Good luck, my friends.
Delicious and Safe: What We Feed Our Child with Eosinophilic Esophagitis
This question is precisely why I founded this blog! While I strive to minimize overly informational posts here, keeping the focus primarily on practical recipes, I often delve into the more personal aspects of our journey on my social media channels. So, be sure to follow me there and watch my stories for real-time updates and insights as they arise. For your culinary needs, I invite you to explore my extensive recipe index, which offers over 200 free recipes, almost all of which are top-8-allergen-free. (A few recipes do include soy, as it is one of the allergens my son can tolerate.)
If you prefer physical copies for your kitchen, I have a published cookbook available for purchase on Amazon. You can discover more details about it, including a full recipe index of its contents, by clicking here, or by clicking on the image of the cookbook below.
Additionally, I’ve created an e-book specifically designed to alleviate the initial stress of dietary changes, featuring two weeks’ worth of top-8-free dinner ideas. The first two weeks can often be the most challenging, so I wanted to provide comprehensive coverage for that period, including a convenient shopping list. Click here to access it, or simply click on the image of the e-book below.
Still Have Questions? Connect With Us!
I understand that managing Eosinophilic Esophagitis can bring up many questions, and I’m committed to providing avenues for further support. My husband and I regularly host live question-and-answer sessions on my Instagram and Facebook pages, where you are always welcome to ask us anything. You can also try emailing me directly, and while I strive to respond to every inquiry, my ability to do so depends on my current volume and workload. Feel free to leave a comment below this post; often, other members of our wonderful community can offer insights and answers based on their own experiences. Additionally, the various links I’ve included throughout this article lead to excellent resources that may help address your specific concerns.
For a deeper dive into many questions readers have asked, here is the live Q&A session we conducted specifically on EoE. It’s almost an hour packed with helpful information and discussions.
DON’T FORGET TO PIN THIS, SO YOU DON’T LOSE IT!


